This is Part 1 of this exciting ECG series. Use the following quick links to navigate to the expert ECG cases quickly:
Stephen Smith’s ECG: 60F with chest discomfort.
Ken Grauer’s ECG: 68M with resolved severe chest pain.
David Didlake’s ECG: 49M with new-onset chest pain.
Nanashi’s ECG: 60M with shortness of breath and fatigue.
1. Stephen Smith (@smithECGBlog)
Background
“This ECG was texted to me by a former resident with no information.”
Only later (after interpretation), Steve received the full clinical story: A 60-something woman with a history of MI and PCI, with 3 hours of chest discomfort. The initial hs troponin was 53 ng/L
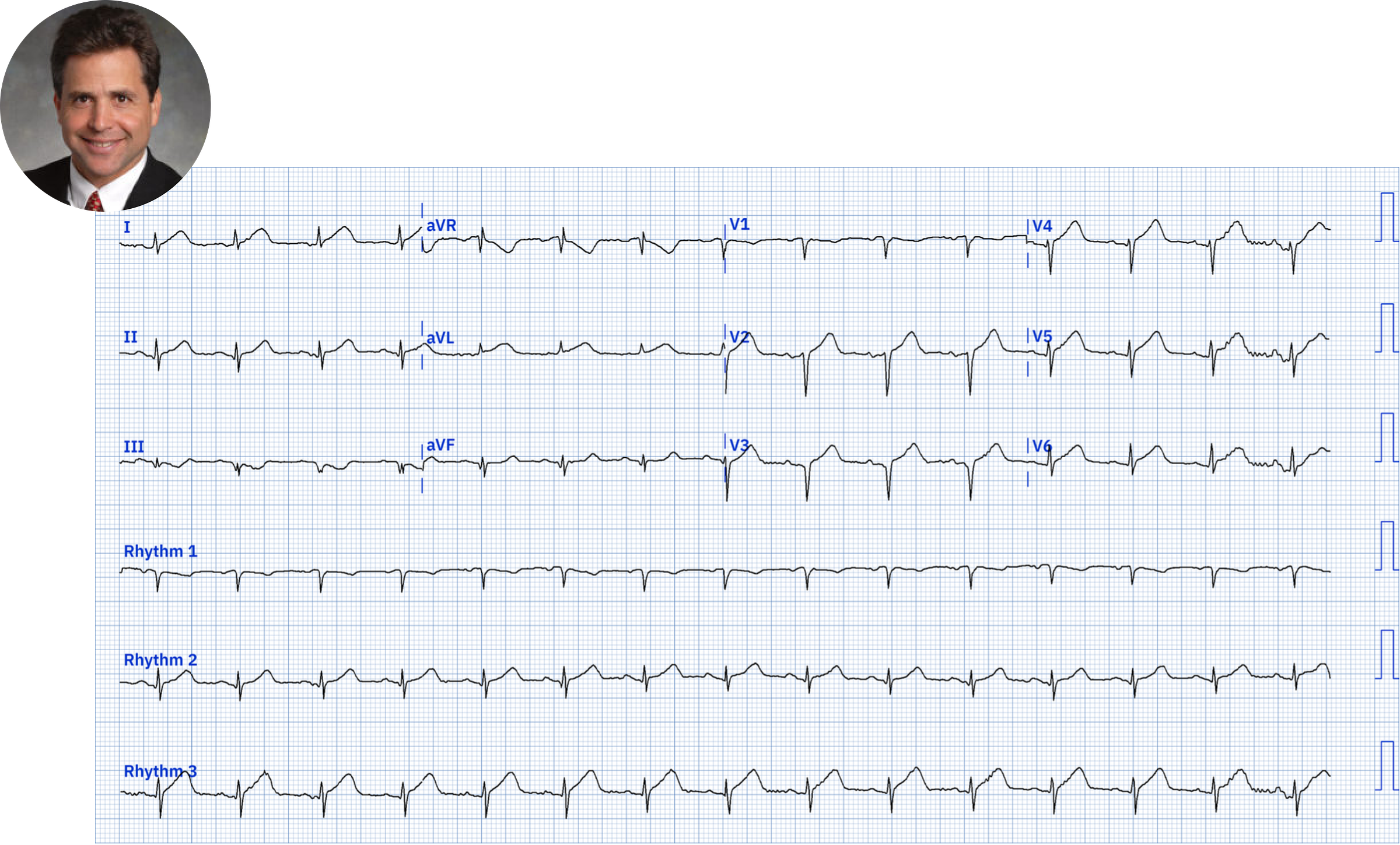
Expert breakdown
This was my immediate response: "Acute proximal LAD OMI" To me it is obvious and diagnostic.
There are hyperacute T-waves in I, aVL, V2-V6. These are wide, bulky, with large area under the curve relative to the QRS size.
Furthermore, there is a QS-wave in V3 and qrS in V4, both diagnostic of MI at some time (past or present). We have shown here and validated here that old MI has a relatively small T-wave (by amplitude). In this situation (QS-waves), a T/QRS ratio >0.36 in any of V1-V4 is highly specific for ACUTE MI.
The former resident then wrote this: "All my colleagues are amazed that I diagnosed this pretty obvious OMI immediately. I didn’t think it was subtle at all but they all say it is."
Check out the original case and the full work up on his blog:
Meet Steve
Dr. Stephen W. Smith is a faculty physician in the Emergency Medicine Residency at Hennepin County Medical Center (HCMC) in Minneapolis, MN, and a Professor of Emergency Medicine at the University of Minnesota. Steve is the founder of Dr. Smith’s ECG Blog and has published several books on ECG interpretation.
2. Ken Grauer (@ekgpress)
Background
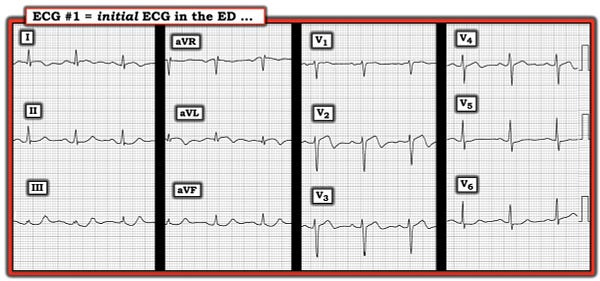
A 68-year-old man with risk factors, presented with severe chest pain lasting ~1 hour — but which resolved by the time he arrived in the emergency department (ED). The patient reports that during the previous week — he experienced 2 similar episodes of severe chest pain, lasting about the same amount of time before spontaneously resolving. This was his initial ECG when arriving pain-free in the ED:
Expert breakdown
The rhythm in ECG #1 is sinus. Regarding intervals — the PR interval and QRS duration are regular; the QTc may be borderline prolonged. There is no chamber enlargement.
Regarding Q-R-S-T Changes:
There are Q waves of uncertain significance in high lateral leads I and aVL.
R wave progression shows slightly delayed transition (the R wave becomes taller than the S wave is deep only between leads V4-to-V5).
The most remarkable findings in relate to ST-T wave Changes:
The ST segment is coved in high-lateral leads I and aVL. There appears to be significant ST elevation in lead aVL — in view of how tiny QRS amplitude is in this lead (which is why the Q wave in lead aVL may be relevant). Relative to QRS amplitude — there is fairly deep and symmetric T wave inversion in lead aVL. Similar ST-T wave changes are seen in lead I — albeit more modest.
The 3 inferior leads (II,III,aVF) — each show similar reciprocal changes with respect to the ST-T wave appearance in lead aVL. (Note terminal positivity of the T wave in each of the 3 inferior leads — with this terminal positive T wave in lead III being taller than the R wave in this lead!).
In the Chest Leads — the most remarkable findings are in lead V2 — which shows straightening of the ST segment — with 1 mm of J-point ST elevation — and a distinct biphasic T wave, with rapid T wave descent into terminal negativity.
The ST-T waves in leads V3,V4 look similar to each other — in that they each manifest ST segment straightening (but no elevation) — and, a hint of terminal T wave negativity.
Lateral chest leads V5,V6 also look similar to each other — and show ST segment straightening, with slight ST depression.
IMPRESSION: The above history, in association with the appearance of the initial ECG in today's case — illustrate the "classic" picture of Wellens' Syndrome.
Here is the link to the full case and interpretation:

Meet Ken
Ken Grauer is Professor Emeritus (Dept. Community Health/Family Medicine, College of Medicine, University of Florida in Gainesville). Dr. Grauer has been a leading family physician educator for over 35 years and has published (as principal author) more than 15 books and numerous study aids on ECG interpretation, cardiac arrhythmias, and ACLS.
RH’s addition: “Ken is highly experienced in ECG interpretation and an active and well-respected member of the EKG Club group on Facebook and Twitter. His annotated ECGs (constructed predominantly in Powerpoint) are well-known pieces of educational content spiking exciting conversations online.
3. David Didlake (@DidlakeDW)
Background
My colleagues and I responded to a 49 y/o Male who called 911 after experiencing new-onset chest discomfort that forced him to pull over while driving. At the time of initial contact, he expressed symptom alleviation and felt that Fire/EMS services were no longer necessary. He at least agreed to a full examination in the ambulance and stated that during its peak the pain was squeezing in nature, centrally located, 8/10 severity, and associated with both diaphoresis and one episode of vomiting.
ASA 324mg was administered. As my colleague was placing the IV catheter the patient leaned forward with Levine sign and expressed chest discomfort with an apparent facial grimace. We immediately captured the following 12-lead at 0901 hours:
Expert breakdown
My gestalt reaction was unequivocal LAD occlusion. There is significant STE V1-V5 with associated Hyperacute T waves (HATW). The HATWs extend to Leads I/aVL, and there is a down-up T wave in aVF. The inverted TW in III is reciprocal to the HATW in aVL. As an aside, it should be noted that the LifePak 15 does not seem too concerned about these changes. Many EMS providers know that when the machine interprets profound shifts to the ST segment, it spontaneously ejects a new tracing with acute injury suspected. This is a testament to the power of provider-directed serial ECGs. A pre-hospital STEMI alert was then transmitted.
This ECG was so pathognomonic to me that I initially didn’t consider it necessary to apply the 4-variable equation for the differentiation of LAD OMI versus Early Repolarization but ultimately decided this imperative as I feared the receiving facility would disregard the changes for reasons soon to be disclosed.
QTc 446 ms
STE 60 ms after the J-point in V3 2 mm
R wave height V4 10 mm
QRS voltage V2 13 mm
Result: 20.67
Check out the initial ECG and the continuation of this excellent case highlighting the dynamics of ACS here:

Meet David
David is a Firefighter / Paramedic and Advanced Practice Registered Nurse (Acute Care NP), interested in all things emergency cardiac care — including ECG interpretation, POCUS, and minimal peri-shock pause cardiopulmonary resuscitation. He actively contributes his excellent ECG cases and highly detailed interpretations on Twitter.
4. Nanashī (@The_Nanashi_O)
Background
Background: Received from a colleague who regularly shares interesting ECG cases with me A man in his 60s with a history of systemic hypertension presented to the Outpatient Department of the hospital in the company of his relatives with complaints of shortness of breath on exertion, fatigue, and reduced exercise tolerance going back 1 week. Prior to these symptoms, he reports experiencing a constant dull substernal chest pain which radiated to the epigastrium and left arm and lingered for a couple of days but was maximal at onset for about 6-8 hours. He did not seek medical attention for unclear reasons and was only convinced to come into the hospital by his concerned relatives.
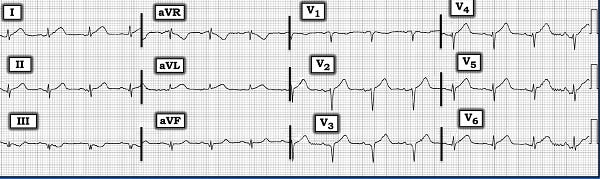
An ECG recorded in the clinic is shown (see image) at which time he was completely pain-free:

Expert breakdown
Rhythm: Upon confirmation of proper lead placement, the rhythm is clearly not sinus but ectopic, possibly from a focus low in the right atrium and close to the AV junction, given the short PR interval. Alternatively, it could be a high junctional escape rhythm.
The mean frontal QRS axis is virtually horizontal (leftward) but within normal range and the QRSd and QTcB are also within normal (86 ms and 410 ms, respectively).
The findings of concern are obviously the unusual ST-T changes. The inferior leads show slight (maybe 0.5 mm) ST elevation followed by downsloping ST segments which continue into deep, large T wave inversions. There is also very healthy R wave voltage in lead II and a reasonably healthy R in aVF. Note the large Q waves in all three inferior leads. ST-T changes in the inferior leads are mirrored in aVL with minimal scooped/coved ST depression leading into an upright T wave.
These changes are altogether suspicious for remote occlusion of a vessel supplying the inferior wall with injury AND spontaneous reperfusion. It is also suggested that there is a significant amount of viable myocardium left given the preserved R waves and large inverted T waves. The chest leads are even more interesting with unexpectedly early R wave progression with what appears to be normal/benign ST elevation in V2-V4 followed by unusually large T waves, relative to the QRS complexes in V2-V4 and conceivably, V5. The tall R waves in V2-V3 are analogous to Q waves of posterior injury and the tall T waves are the anterior mirror representation of reperfusion T waves (so-called posterior Wellens’ T waves) of posterior OMI.
Putting the limb and chest lead findings together; we appear to be looking at an unusual representation of inferior OMI with reperfusion and posterior OMI with reperfusion. This interpretation would not be prudent to make without the benefit of a knowledge of the timing of events surrounding the ECG. He was referred to the cardiology service and it is unclear what the outcome was.
Meet Nanashī
Nanashī is a physician in the United Kingdom with an interest in emergency electrocardiography, acute MI and cardiac disarrythmias. While his identity remains unknown, he is an active contributor to the ECG interpretation community on Twitter.
BONUS
Here are the automatic AI-powered interpretations generated for these 4 exciting cases. Interestingly the Wellens’ pattern in Ken’s case was detected with a lower ACS patient priority than the Wellens’ T waves in Nanashi’s case. Suspected ST-elevation ACS here is the equivalent of immediate cathlab activation in the context of acute coronary occlusion.
Robert Herman, MD is a physician and scientist with a background in technology and expertise in AI and machine learning. He is the Co-founder of Powerful Medical, where he serves as the Chief Medical Officer and leads the research and clinical evaluation of AI-powered medical devices for diagnosing and managing cardiovascular diseases.
If you liked this, please click the🤍 below so other people will see this here on Substack and consider sharing the article.







When does the United States PMcardio app get released? Does anyone know?
Great cases!